Nearly 1 in 3 blood cancer patients and survivors say they are unlikely to get a COVID-19 vaccine, or unsure about it, despite their heightened risk
RYE BROOK, N.Y., March 8, 2021 – A new survey of more than 6,500 U.S. blood cancer patients and survivors reveals that only half are very likely to get a COVID-19 vaccine while one in three is either unlikely or unsure about it. The nationwide survey was a collaboration between The Leukemia & Lymphoma Society (LLS), Boston University Questrom School of Business, and The Behaviouralist, a London-based research consultancy.
The results come despite the serious risks facing blood cancer patients. Some early studies suggest around half of blood cancer patients hospitalized with COVID-19 will die from the disease.
“These findings are worrisome, to say the least,” said Gwen Nichols, M.D., LLS Chief Medical Officer. “We know cancer patients – and blood cancer patients, in particular – are susceptible to the worst effects of this virus. All of us in the medical community need to help cancer patients understand the importance of getting vaccinated.”
“Blood cancer patients are being given preferential access to limited vaccine supplies in many communities, but that doesn’t mean they are willing and able to get vaccinated,” said Rena Conti, Dean’s Research Scholar and Associate Professor at Boston University Questrom School of Business. “We need both adequate supply and strong demand to keep this vulnerable population safe.”
The survey is the largest to date asking cancer patients and survivors about their attitudes towards COVID-19 vaccines.
There have been widespread reports that cancer patients and survivors across the country have struggled to obtain the vaccine. The newly-released survey results add another wrinkle to that story: a large portion of cancer patients may not feel comfortable getting the vaccine, even if it’s made available to them.
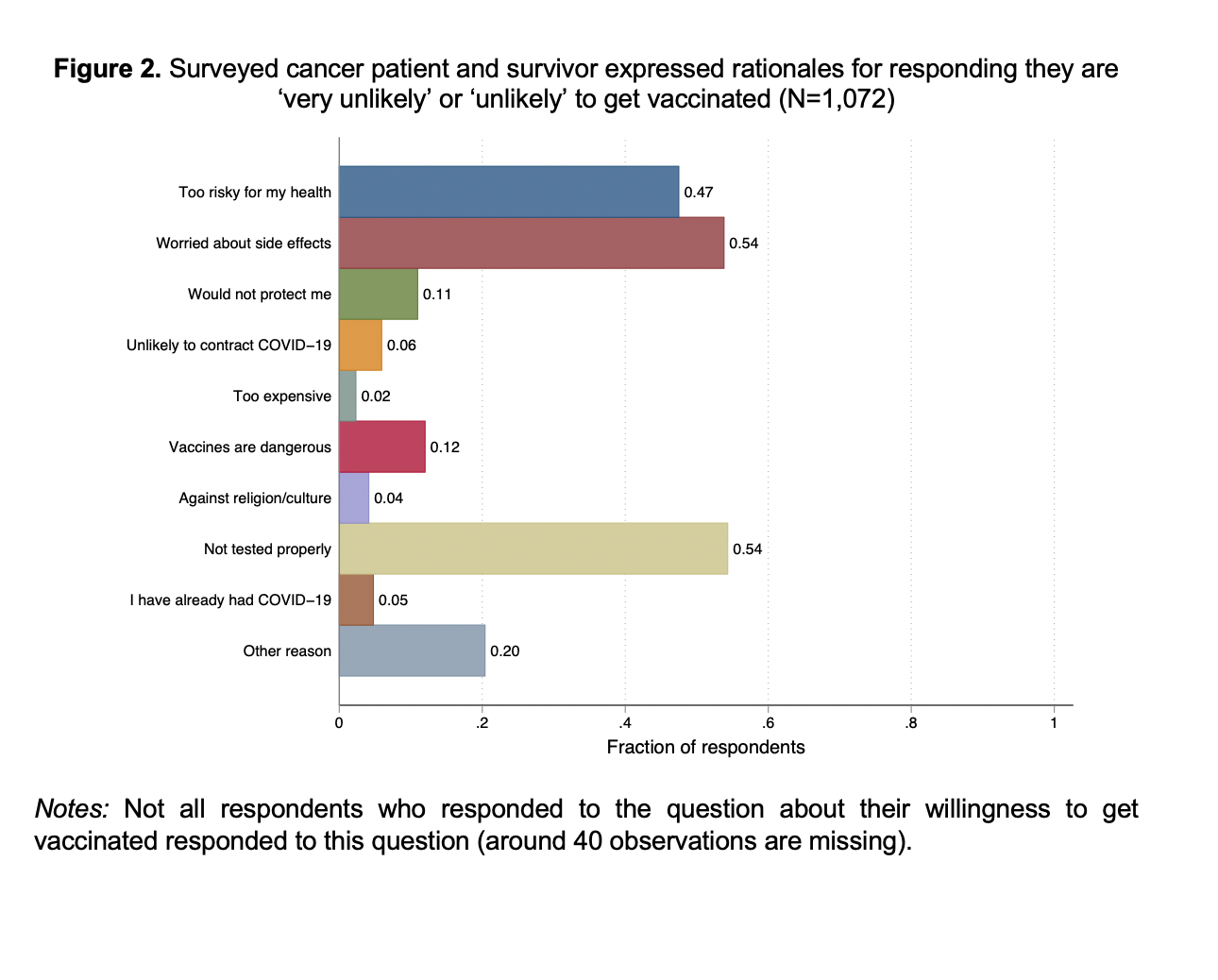
The most common reasons cited for hesitancy were concerns about side effects and a belief that the vaccines have not been tested properly. There is no reason to believe COVID-19 vaccines are any less safe in patients with blood cancers. There are concerns, however, that patients with some types of blood cancer or undergoing certain treatments may not mount the same immune response from the vaccine as the general public. Cancer patients were largely excluded from COVID-19 vaccine trials.
LLS has launched the LLS National Patient Registry, open to anyone with blood cancer, to help answer important questions about vaccine effectiveness.
“Right now, we’re missing key data – and patients know it,” Nichols said. “That may be one of the reasons they’re skeptical. By improving our understanding of how blood cancer patients and survivors respond to these vaccines, we can develop better strategies to protect them from COVID-19.”
LLS also plans to repeat the survey soon to assess cancer patients’ and survivors’ evolving access to vaccines and willingness to get vaccinated. This effort will help improve future educational and outreach efforts to this vulnerable community.
In the meantime, LLS advises blood cancer patients to discuss vaccination with their oncologist and healthcare team as soon as possible so they can make an informed plan of action when a vaccine becomes available to them. Well over 100 leading cancer organizations have underscored the urgency of prioritizing vaccine access for cancer patients and survivors, and CDC guidelines prioritize cancer patients in the “1c” vaccination group.
About the Survey
Patients and survivors included in The Leukemia & Lymphoma Society’s database were surveyed during the first three weeks of December 2020. During that time, the U.S. Food and Drug Administration granted Emergency Use Authorization to both the Moderna and Pfizer–BioNTech COVID-19 vaccines.
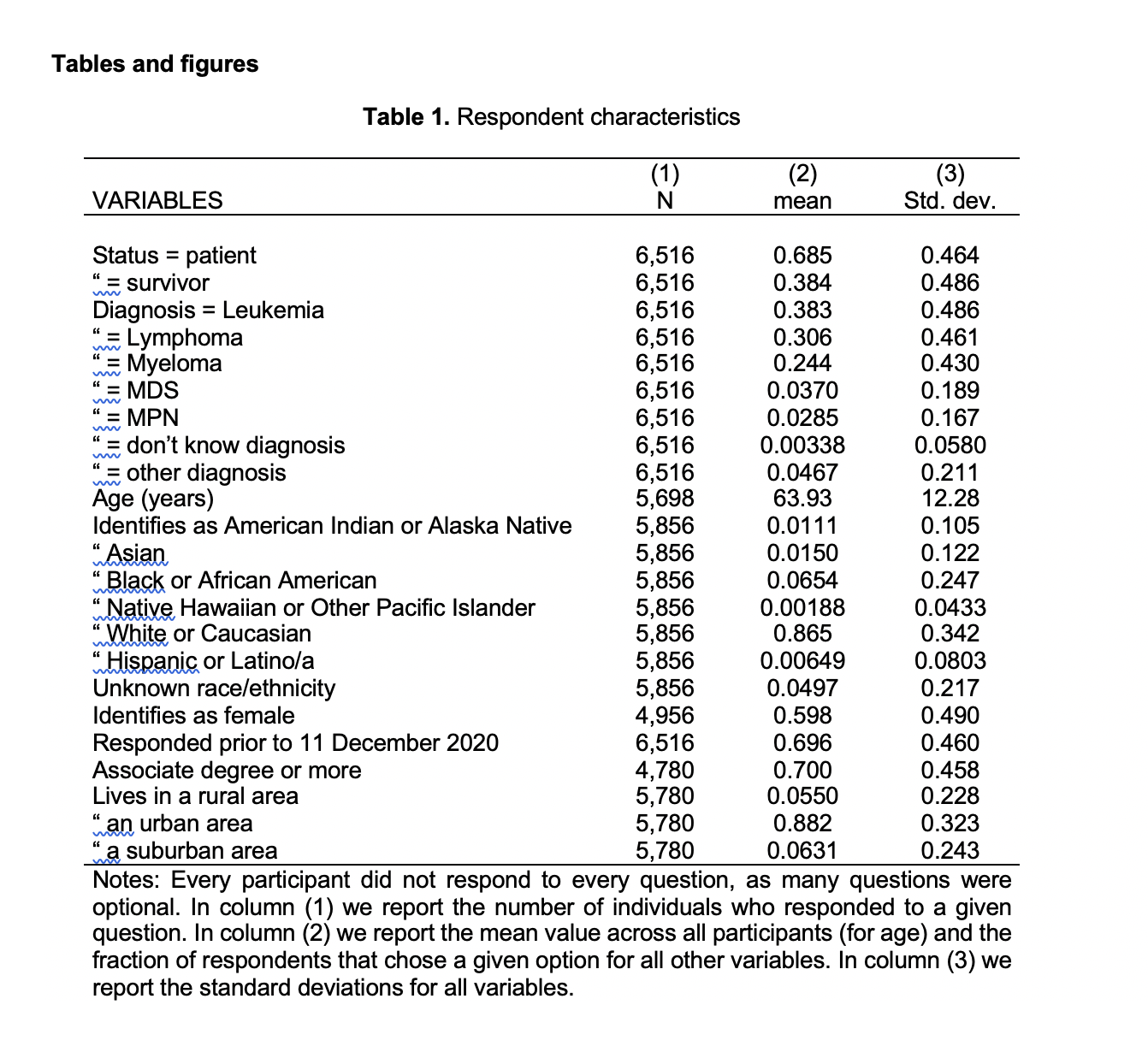
Six in 10 (59.8%) of the 6,516 respondents were female, 86% identified as white, 6.5% as Black or African American and 4.7% as Hispanic or Latino/a. The average age of the respondents was 64 years and most (70%) had an Associate’s degree or more.
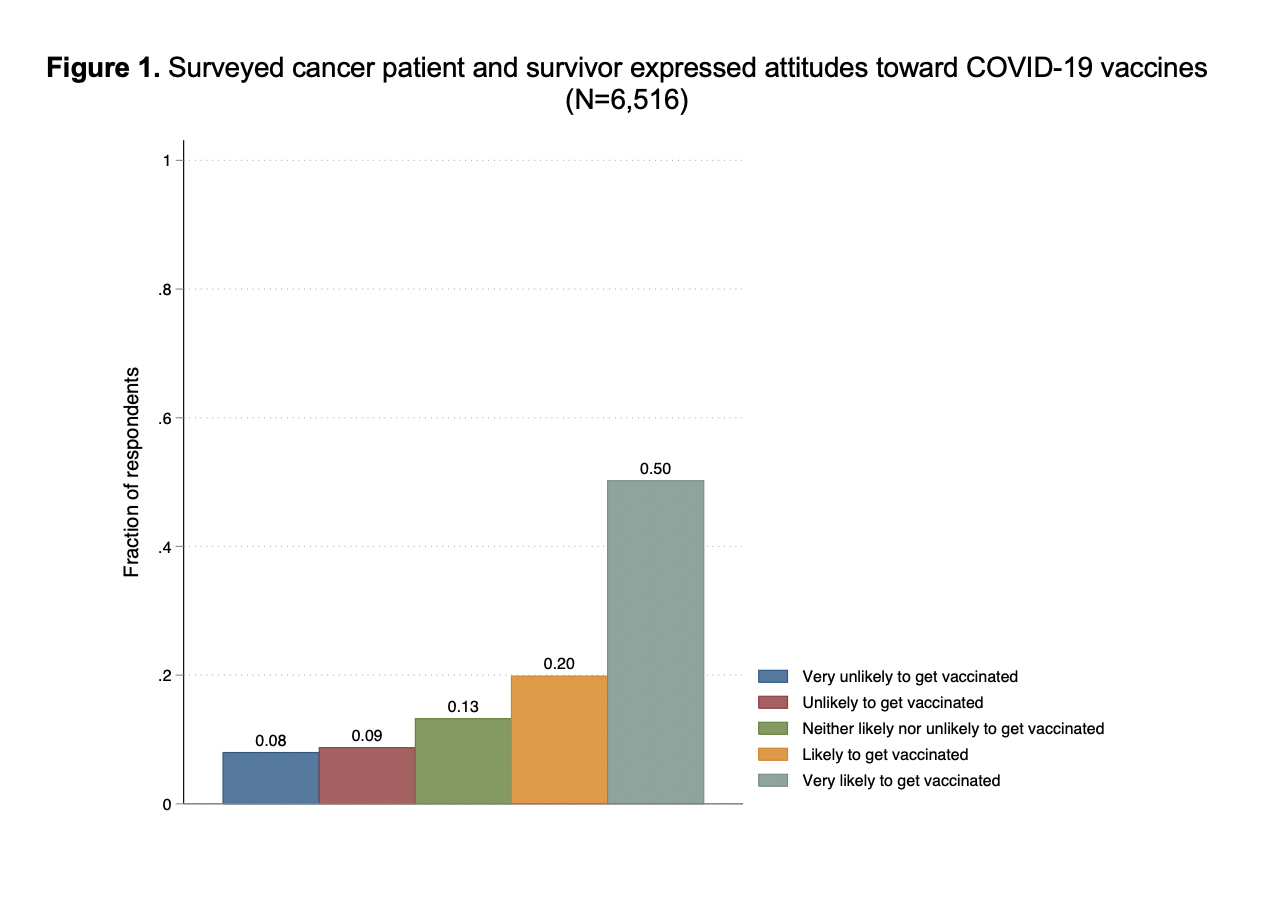
Seventy percent said they are either very likely (50%) or likely (20%) to get the COVID vaccine. The remaining 30% said they are very unlikely (8%), unlikely (9%) or neither likely nor unlikely to get vaccinated (13%).
About The Leukemia & Lymphoma Society
The Leukemia & Lymphoma Society® (LLS) is a global leader in the fight against cancer. The LLS mission: cure leukemia, lymphoma, multiple myeloma, and improve the quality of life of patients and their families. LLS funds lifesaving blood cancer research around the world, provides free information and support services, and is the voice for all blood cancer patients seeking access to quality, affordable, coordinated care.
Founded in 1949 and headquartered in Rye Brook, NY, LLS has regional offices throughout the United States and Canada. To learn more, visit www.LLS.org. Patients should contact the LLS Information Resource Center at (800) 955-4572, Monday through Friday, 9 a.m. to 9 p.m., ET.
For additional information visit lls.org/lls-newsnetwork. Follow us on Facebook, Twitter, and Instagram.
About Boston University
Founded in 1839, Boston University is an internationally recognized institution of higher education and research. With more than 34,000 students, it is the fourth-largest independent university in the United States. BU consists of 17 schools and colleges, along with the Faculty of Computing & Data Sciences and a number of multi-disciplinary centers and institutes integral to the University’s research and teaching mission. In 2012, BU joined the Association of American Universities (AAU), a consortium of 65 leading research universities in the United States and Canada.
About The Behaviouralist
The Behaviouralist is a research consultancy specializing in understanding, and changing, human behavior. Founded in 2014 by professors Robert Metcalfe and Robert Hahn, the team at The Behaviouralist has worked with governments, utility companies, charities, and other organizations on challenges related to public health, resource conservation, tax compliance, sustainable transportation, and workplace productivity. For more information, please visit www.thebehaviouralist.com.
Media Contacts:
Ryan Holeywell
The Leukemia & Lymphoma Society
ryan.holeywell@lls.org
(202) 277-0802
Michael Sherry
Belfort Group (on behalf of Boston University)
Mike@thebelfortgroup.com
(617) 646-3318 (Direct)
(201) 615-2218 (Mobile)
Jesper Akesson
The Behaviouralist
jesper@thebehaviouralist.com
+44 7554 370 524
Survey Abstract: COVID-19 vaccine hesitancy among blood cancer patients
March 2, 2021
Rena Conti1, Jesper Akesson2, Elisa Weiss3, Maria Sae-Hau3, Marialanna Lee3, Gabriela Gracia4, Brian Connell3, Lucy Culp3, Robert Metcalfe1,2
1 Boston University, Boston, MA
2 The Behaviouralist, London, UK
3 The Leukemia & Lymphoma Society, Rye Brook, NY
4 Independent Researcher
Context
Cancer patients, and specifically those with blood cancer, are among the most vulnerable to disruptions in care and poor outcomes associated with COVID-19 infection.1,2,3 January 2021 CDC guidelines prioritize cancer patients in the ‘1c’ vaccine group based on this evidence.4 National clinical practice guidelines5 and noted physician advocacy groups6 recommend that blood cancer patients get vaccinated, suggesting that the expected benefits outweigh the risks. However, we do not know the extent to which cancer patients demonstrate vaccine hesitancy.∗
Objectives
We conducted a nationwide online survey of blood cancer patients and survivors about their experiences and attitudes related to COVID-19 and COVID-19 vaccines, using a convenience sample of blood cancer patients and survivors with valid email addresses who are in The Leukemia & Lymphoma Society’s constituent database. In total, 6,516 patients and survivors responded to the survey, for a response rate of nearly 7%.
Methods
The main outcome is vaccine attitudes, specifically respondents’ answers to the question: ‘Imagine that your doctor offers you a COVID-19 vaccine for free in January 2021. How likely are you to choose to get the vaccine?’ scored on a five-point Likert scale (very unlikely, unlikely, neither likely nor unlikely, likely, and very likely). Rationales for answers to this question were recorded and categorized. We also asked respondents: 1) whether and how COVID-19 impacted their medical care, finances, and social support; 2) about their COVID-19-related beliefs and engagement with protective health-related behaviors (e.g., wearing a mask or washing their hands frequently); and 3) about their demographic characteristics. The survey was fielded between December 1-21, 2020.
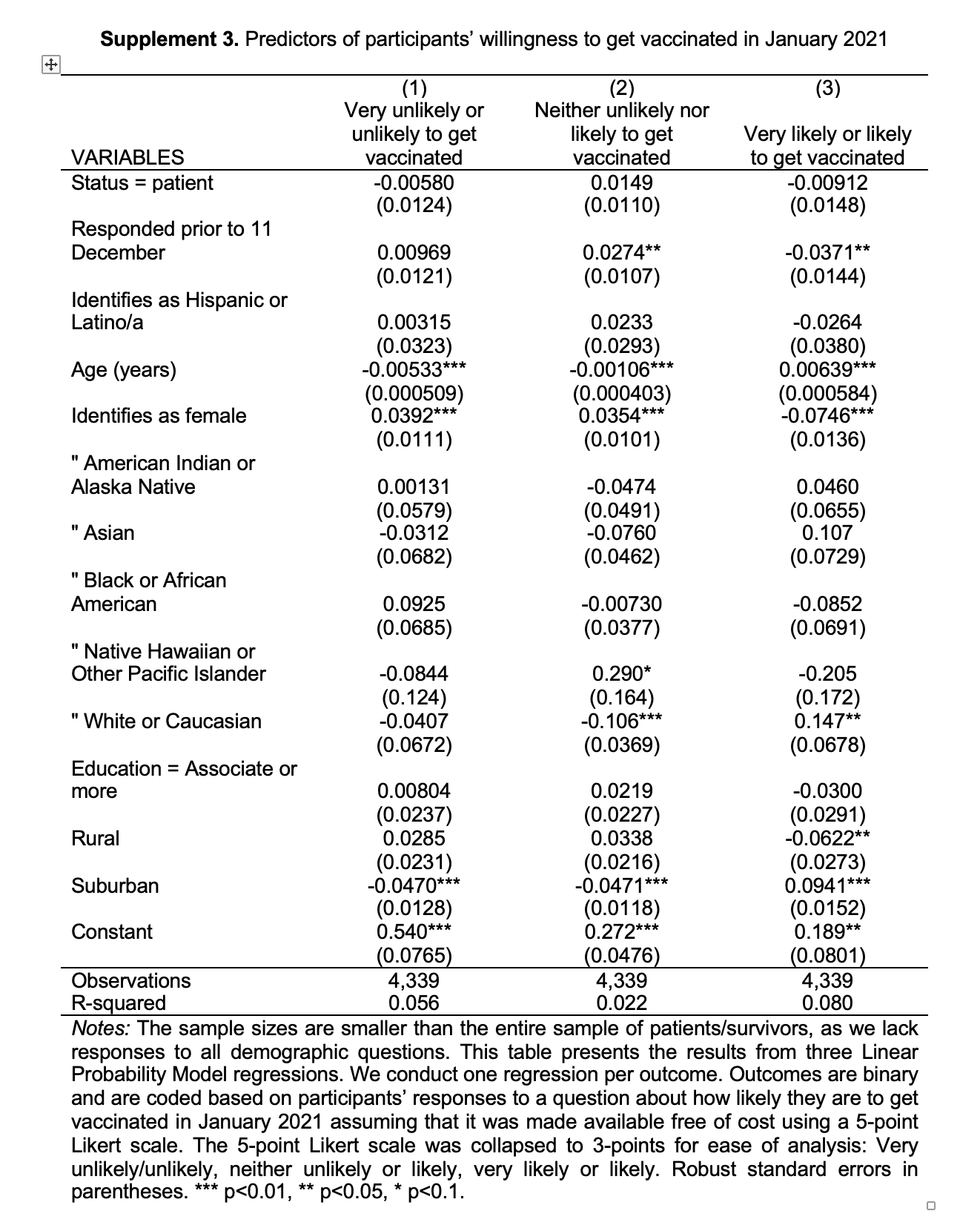
We present mean responses to the main outcome. We conduct t-tests of differences in proportions to evaluate how vaccine attitudes are related to other health beliefs and behaviors. We also conduct three Linear Probability Model (LPM) regressions to correlate participants’ vaccine attitudes with other observable variables (e.g., their demographic characteristics and whether they responded to the survey before or after the Pfizer-BioNTech and Moderna vaccines had been emergency authorized in the US [beginning 10 December 2020]).8,9 The outcomes for these regressions are three binary variables. The first variable takes the value of one if the respondent is ‘very unlikely’ or ‘unlikely’ to take a vaccine, and zero otherwise. The second variable takes the value of one if the respondent is ‘neither likely nor unlikely’ to take a vaccine, and zero otherwise. The third variable takes the value of one if the respondent is ‘likely’ or ‘very likely’ to take a vaccine, and zero otherwise. We verify the robustness of the regression results by estimating a multinomial logit model and by re-weighting the data so that the population better reflects the overall population of blood cancer patients in the US (by re-weighting on race/ethnicity, gender, and age). We only report results that are statistically significant on a 5% level. We use the statistical software Stata (version 16) to conduct the data analysis. The Institutional Review Board of Boston University approved this study.
Results
The average age of respondents is 64, 59.8% are female, and 70% have an Associate degree or more (Table 1). Further, 86.5% identify as White or Caucasian, 6.5% identify as Black or African American, and 4.7% identify as Hispanic or Latino/a.
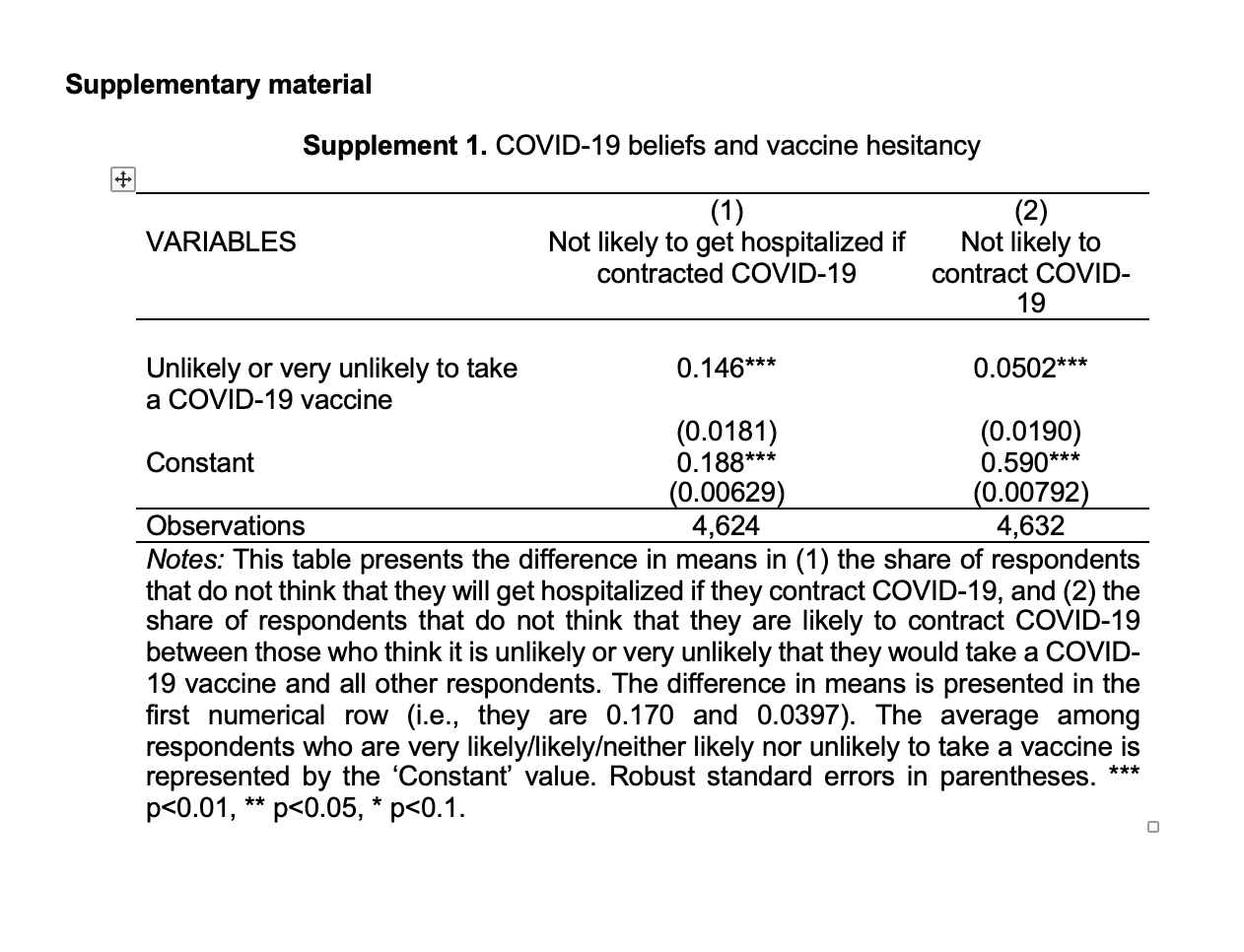
We find that 17% of respondents indicate that they are unlikely or very unlikely to take a vaccine (Figure 1). Among those who are vaccine hesitant (i.e., those that state that they are ‘unlikely’ or ‘very unlikely’ to get vaccinated), the two most common reasons (both 54%) are concerns regarding side effects and a belief that the vaccines “will not be/have not been tested properly” (Figure 2). Relative to other respondents, those who are vaccine hesitant are significantly (14.6 percentage points) more likely to say that they do not think they would get hospitalized if they contracted COVID-19 (Supplement 1). They are also significantly (5 percentage points) more likely to say that they do not think they will contract COVID-19.
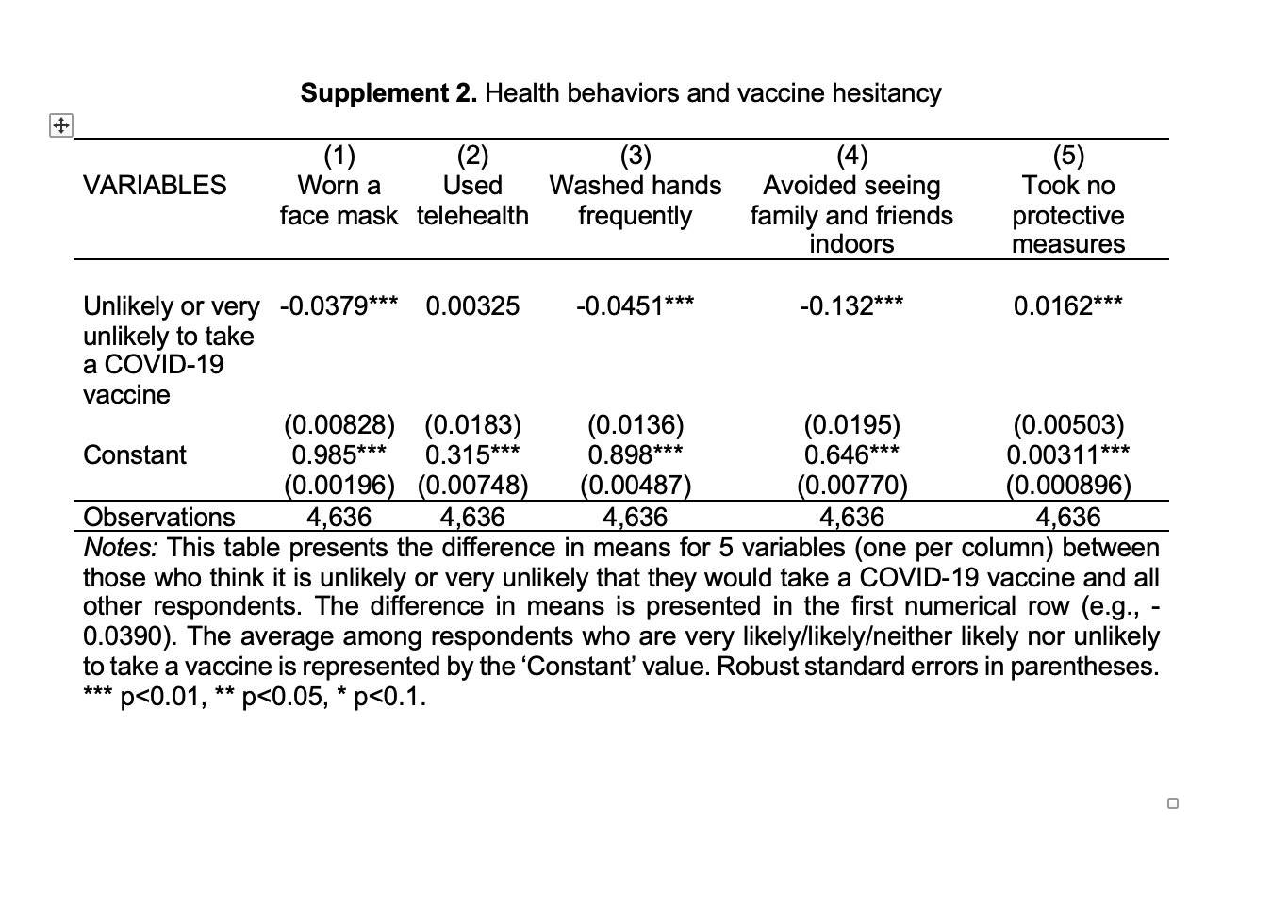
Vaccine hesitant respondents are also significantly less likely to engage in protective health behaviors (Supplement 2). They are, for example, 3.8 percentage points less likely to say that they have worn a face mask and 1.6 percentage points more likely to say that they have taken no other protective measures.
None of the aforementioned results change appreciably when re-weighting the data (for age, gender, and race/ethnicity) or using alternative statistical specifications.
Limitations
It is unknown whether these results generalize to wider groups of cancer patients or racial and ethnic populations underrepresented in the survey population or those with lower levels of education (although our re-weighted analysis suggests that the results do generalize). It is also not clear how stated intentions to take a COVID-19 vaccine translate into actual vaccination behavior.10-12
Discussion
We conducted the largest and most timely survey of cancer patient and survivor attitudes, experiences, and behaviors related to COVID-19. We found that a little less than one in five cancer patient and survivors report vaccine hesitancy. The most frequent rationales for vaccine hesitancy are consistent with the fact that the currently available vaccines were not tested on these patient types (cancer patients and survivors were excluded from the trials), but inconsistent with recent recommendations of public health and cancer experts who believe the benefits of vaccination outweigh the risks.13
Our finding regarding the prevalence of vaccine hesitancy can be compared to that of the Kaiser Family Foundation (KFF) survey fielded coincidently at about the same time in December 2020, which reported lower rates of vaccine hesitancy. KFF found that 71% of the general population would definitely or probably get vaccinated if it were determined to be safe by scientists and available for free vs. 70% among our sample respondents. KFF also found that among households in which someone had a serious health condition (defined to include cancer), 78% would definitely or probably get vaccinated.14 While it may be surprising that our figure is slightly lower than these estimates (given the more significant risks of morbidity and mortality among blood cancer patients who contract COVID-19), the greater degree of hesitancy among blood cancer patients may also reflect greater underlying uncertainty regarding not only the safety but also the efficacy of COVID-19 vaccines for this specific population. In fact, although national guidelines and physician groups recommend that blood cancer patients be vaccinated, they note that the efficacy (i.e., the degree to which cancer patients develop immunity when vaccinated) is unknown, and there is concern that patients with a blood cancer will have a lower immune response than the general public.5
We also found that participants became more positive toward taking a COVID-19 vaccine once the FDA had approved the Pfizer-BioNTech and Moderna vaccines. This suggests that hesitancy may be influenced by emerging information dissemination, government action and vaccine availability, transforming the hypothetical opportunity of vaccination to a real one.
Policy implications
Patients, physicians and policymakers need data on the effectiveness of COVID-19 vaccines in cancer patients to inform practice. To overcome vaccine hesitancy, clear, consistent and culturally appropriate messaging targeting cancer patients, emphasizing the risks of COVID-19 infection and the benefits of vaccination may be needed. It is also important to increase diversity of participants in COVID-19 vaccine trials, so that participants are from communities most impacted by the virus.15 Guidelines might also consider the benefits of offering vaccinations to caregivers of cancer patients to reduce COVID-19 transmission and improve access to care.
∗Vaccine hesitancy, according to the World Health Organization, is the “delay in acceptance or refusal of safe vaccines despite availability of vaccination services.”7
References
- Bakouny Z, Hawley JE, Choueiri TK, et al. COVID-19 and cancer: current challenges and perspectives. Cancer Cell. 2020;38(5):629-646.
- Banks MA. COVID-19 more deadly with blood than solid cancer: study. The Scientist. Published February 16, 2021. Accessed March 2, 2021. https://www.the-scientist.com/news-opinion/covid-19-more-deadly-with-blood-than-solid-cancer-study-68459
- Vijenthira A, Gong IY, Fox TA, et al. Outcomes of patients with hematologic malignancies and COVID-19: a systematic review and meta-analysis of 3377 patients. Blood J Am Soc Hematol. 2020;136(25):2881-2892.
- Evidence used to update the list of underlying medical conditions that increase a person’s risk of severe illness from COVID-19. Centers for Disease Control and Prevention. Published November 2, 2020. Accessed January 27, 2021. https://www.cdc.gov/coronavirus/2019-ncov/need-extra-precautions/evidence-table.html
- National Comprehensive Cancer Network. Preliminary Recommendations of the NCCN COVID-19 Vaccination Advisory Committee*. Published online January 22, 2021. Accessed January 27, 2021. https://www.nccn.org/covid-19/pdf/COVID-19_Vaccination_Guidance_V1.0.pdf
- COVID-19 Vaccine & Patients with Cancer. American Society of Clinical Oncology. Published January 15, 2021. Accessed January 27, 2021. https://www.asco.org/asco-coronavirus-resources/covid-19-patient-care-information/covid-19-vaccine-patients-cancer
- Vaccine hesitancy: A growing challenge for immunization programmes. World Health Organization. Published August 18, 2015. Accessed February 1, 2021. https://www.who.int/news/item/18-08-2015-vaccine-hesitancy-a-growing-challenge-for-immunization-programme
- COVID-19 Vaccines. U.S. Food and Drug Administration. Accessed January 27, 2021. https://www.fda.gov/emergency-preparedness-and-response/coronavirus-disease-2019-covid-19/covid-19-vaccines
- Frequently Asked Questions about COVID-19 Vaccination. Centers for Disease Control and Prevention. Published January 25, 2021. Accessed January 27, 2021. https://www.cdc.gov/coronavirus/2019-ncov/vaccines/faq.html
- Harris KM, Maurer J, Lurie N. Do people who intend to get a flu shot actually get one? J Gen Intern Med. 2009;24(12):1311. doi:https://doi.org/10.1007/s11606-009-1126-2
- Nowak GJ, Cacciatore MA, Len-Ríos ME. Understanding and Increasing Influenza Vaccination Acceptance: Insights from a 2016 National Survey of U.S. Adults. Int J Environ Res Public Health. 2018;15(4):711. doi:https://doi.org/10.3390/ijerph15040711
- Bronchetti ET, Huffman DB, Magenheim E. Attention, intentions, and follow-through in preventive health behavior: Field experimental evidence on flu vaccination. J Econ Behav Organ. 2015;116:270-291. doi:https://doi.org/10.1016/j.jebo.2015.04.003
- Dooling K, Marin M, Wallace M, et al. The Advisory Committee on Immunization Practices’ Updated Interim Recommendation for Allocation of COVID-19 Vaccine — United States, December 2020. U.S. Department of Health and Human Services/Centers for Disease Control and Prevention; 2021:1657-1660. Accessed January 27, 2021. http://www.cdc.gov/mmwr/volumes/69/wr/mm695152e2.htm?s_cid=mm695152e2_w
- Hamel L, Kirzinger A, Munana C, Brodie M. KFF COVID-19 Vaccine Monitor: December 2020. Kaiser Family Foundation; 2020. Accessed January 25, 2021. https://www.kff.org/coronavirus-covid-19/report/kff-covid-19-vaccine-monitor-december-2020/
- Zhang AD, Puthumana J, Egilman AC et al. Demographic Characteristics of Participants in Trials Essential to US Food and Drug Administration Vaccine Approvals, 2010–2020. J Gen Inern Med, 2021; March 3. https://doi.org/10.1007/s11606-021-06670-3.